All published articles of this journal are available on ScienceDirect.
Primary Syphilitic Chancre Presenting as a Non-healing Ulcer of the Lower Lip: A Case Report
Abstract
Introduction
The diagnosis of primary syphilis can be challenging, as direct inoculation at non-genital sites such as the lips may result in extragenital chancres, even though the disease typically presents as a genital ulcer.
Case Presentation
A 32-year-old man had a lower lip ulcer that was indurated and painless for three weeks. The patient reported a history of orogenital contact with a woman 17 days before the appearance of the lip ulcer. Initially, the lesion was misdiagnosed as a traumatic ulcer and was unsuccessfully treated with topical antibiotics. Examining the lower lip revealed a single, distinct, oval ulcer with a clean base and firm induration. The submental lymph nodes showed a slight non-tender enlargement.
A confirmatory Treponema Pallidum Hemagglutination Assay (TPHA) and a positive Venereal Disease Research Laboratory (VDRL) test (1/64) were found through serological testing. Human Immunodeficiency Virus (HIV) and Herpes Simplex Virus immunoglobulins (HSV IgM, IgG) were not detected. After receiving a single intramuscular dose of 2.4 million units of benzathine penicillin G, the patient recovered completely in two weeks.
Conclusion
Chronic indurated ulcers of the lip may have various etiologies, and the possibility of a primary syphilitic chancre, though rare, should always be considered. Awareness of this presentation is essential, as early diagnosis and appropriate treatment are crucial to prevent disease progression and transmission.
1. INTRODUCTION
Syphilis, caused by the bacterium Treponema pallidum subsp. pallidum (TPA) is a common sexually transmitted infection that can have serious long-term consequences if left untreated. Syphilis is widely believed to have caused a large epidemic in Renaissance Europe after previously being absent or unrecognized [1].
Although the origins of syphilis and the precise dating of the most recent common ancestor of TPA are still debated [2-4], it is suggested that the strains of TPA that remain in human populations today can be traced back to its introduction into Western Europe around 500 years ago and subsequent global spread [3, 4].
Typically, the syphilitic chancre is a single entity. The tissue in the center is bright red, surrounded by shallow, ill-defined erosions and a firm, indurated base. It has a film layer that resembles polish on which the serosity forms. This characteristic appearance makes it distinguishable from other skin lesions. Early recognition and treatment are crucial to prevent the progression of the infection and avoid serious complications [5].
2. CASE PRESENTATION
A 32-year-old man had a single lower lip ulcer that had been present for three weeks. The patient reported a history of orogenital contact with a woman 17 days before the appearance of the lip ulcer. A tiny papule at the start of the lesion eventually developed into an ulcer. There was no bleeding, no pain, and no systemic symptoms connected to the ulcer. There was no prior history of lip biting, trauma, or comparable lesions elsewhere.
Examining the lateral side of the lower lip revealed a single, distinct ulcer that measured 1.5×1 cm with clean bases and indurated edges (Fig. 1). The submental lymph nodes showed a slight non-tender enlargement. Examinations of the genital area and oral cavity revealed nothing unusual.
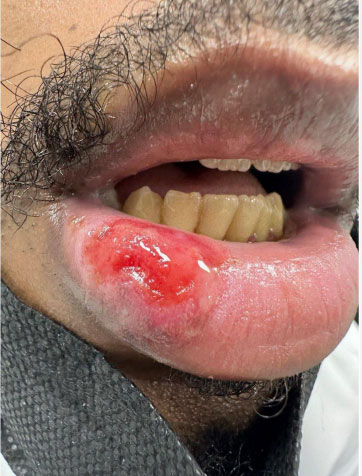
Shows painless well defined indurated single ulcer on the lateral side of the lower lip.
Routine blood investigations were normal. Serology showed VDRL positive 1:64 and TPHA positive. HIV, HSV IgM, IgG, and hepatitis B/C serology were negative. The diagnosis of primary syphilitic chancre of the lip was established based on clinical and serological results.
The patient received a single intramuscular dose of 2.4 million units of benzathine penicillin G, along with screening and partner notification instructions. At the two-week follow-up, the ulcer was fully epithelialized (Fig. 2). After 3 months, the VDRL titre decreased 4-fold.
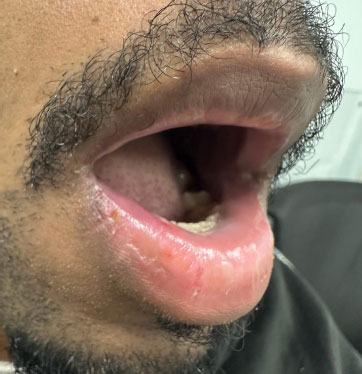
Showed complete healing of the labial syphilitic chancre after 2 weeks treatment with 2,4 million units of benzathine penicillin.
3. DISCUSSION
Syphilis is a sexually transmitted infection caused by Treponema pallidum (TP), and its prevalence has increased dramatically worldwide in recent years [5, 6].
The clinical presentation of syphilis varies widely, even though it is generally described as progressing through primary, secondary, latent, and tertiary stages, after an incubation period of roughly 21 days [7]. Extragenital chancres can vary in terms of location, number, size, shape, ulcer depth, base, edge characteristics, and subjective complaints. They can appear anywhere, including the lip, tongue, palate, face, eyes, neck, trunk, nipples, palmar surface, and fingertips. However, 40-70% of extragenital chancres are found in the oral area, with half of them on the lips [5].
Several reports have highlighted the diagnostic challenges associated with this uncommon form of syphilis. Huang et al. reported that a nonspecific ulcer on the upper lip may present as the first and sole manifestation of primary syphilis [8]. Porterfield et al. also reported a case of a lower lip chancre presenting as a chronic non-healing ulcer that was initially unresponsive to antibiotic therapy before syphilis was confirmed histologically and serologically [9]. Ficarra and Carlos also reviewed multiple oral syphilis cases and found that misdiagnosis and delayed treatment are common due to the disease's various oral presentations [10].
Extragenital chancres on the lips may appear atypically, resembling impetigo, traumatic ulcers, herpes labialis, squamous cell carcinoma, leishmania, cheilitis, lichen planus, drug reactions, Behcet disease, bullous diseases, ulcers caused by Epstein-Barr virus and/or cytomegalovirus, deep fungal infections, or cutaneous tuberculosis [11, 12].
All of the aforementioned differential diagnoses were carefully excluded after a thorough history, clinical examination, and appropriate laboratory tests. A traumatic ulcer was ruled out because there was no history of mechanical injury, such as lip biting, sharp teeth, or dental appliances, and such ulcers are usually painful, with irregular margins and an erythematous base. Herpes labialis was ruled out because there were no painful, grouped vesicles or recurrent shallow ulcers, and serological tests for herpes simplex virus were negative. Chancroid was ruled out because the ulcer was painless, firm, and indurated, as opposed to the soft, painful, ragged ulcers of Haemophilus ducreyi, and there was no associated tender suppurative lymphadenopathy. Aphthous ulcer was ruled out due to the lack of pain, recurrent episodes, and the characteristic shallow ulcers with a yellow base and erythematous halo. Cutaneous tuberculosis was ruled out due to the lack of systemic symptoms such as fever or weight loss, as well as the lesion's non-tender and indurated nature, but no histopathological examination or acid-fast bacilli stains were performed. Deep fungal infection was ruled out because there was no history of chronic indurated ulceration or regional lymphadenopathy indicative of such infections. Since the lesion lacked the hallmarks of malignancy, such as rolled, everted edges, a propensity to bleed, squamous cell carcinoma was also ruled out.
Our case was confirmed based on these findings, as well as a single, painless, indurated ulcer with a clean base, firm, non-tender regional lymphadenopathy, and positive serological tests for Treponema pallidum.
4. STUDY LIMITATIONS
The limitation of this study is the lack of a tissue biopsy from the lip.
CONCLUSION
Primary syphilitic chancre on the lip, while uncommon, should be considered in the differential diagnosis of any chronic, indurated lip ulceration. Awareness of this presentation helps prevent misdiagnosis and ensures timely treatment.
AUTHORS’ CONTRIBUTIONS
It is hereby acknowledged that all authors have accepted responsibility for the manuscript's content and consented to its submission. They have meticulously reviewed all results and unanimously approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| TPHA | = Treponema Pallidum Hemagglutination Assay |
| VDRL | = Venereal Disease Research Laboratory |
| TP | = Treponema Pallidum |
CONSENT FOR PUBLICATION
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
ACKNOWLEDGEMENTS
Declared none.


